Introduction
Imagine a world where damaged hearts can be mended, where blindness might be reversed, or where diseases like Parkinson’s could be slowed or even stopped — not with traditional drugs or surgery, but by using the body’s own building blocks. This is not science fiction; this is the emerging reality of cell therapy, one of the most exciting frontiers in modern medicine.
In this article, we’ll explore what cell therapy is, how it works, and the real hope it offers for people facing a wide range of serious illnesses. We’ll keep things simple and focus on the big picture of what it means for patients, families, and the future of healthcare.
What Is Cell Therapy?
At its core, cell therapy means treating disease by restoring or altering certain sets of cells or by injecting healthy new cells into the body. The idea is that, by giving the body new or modified cells, we can repair or replace tissues that aren’t working properly. Think of it like replacing a broken spark plug in a car engine. Instead of trying to patch it up, you simply swap it out with a new one, and the engine runs smoothly again. In cell therapy, the “spark plugs” are cells—the basic building blocks of our bodies—and scientists are finding ways to grow, engineer, or reintroduce them to help people heal from disease.

Every part of your body — your heart, skin, brain, muscles — is made of cells, trillions of them, each with specific functions. When cells are damaged, diseased, or missing, your body can suffer.
Some cells in the body are constantly growing and replicating, such as your skin and gut cells but in many conditions, like heart failure or spinal cord injury, the body doesn’t naturally regrow the cells it has lost. That’s where cell therapy comes in.
There are many types of cells used in cell therapy, examples being:
Stem Cells
These are special cells that can turn into many different types of cells (like heart, nerve, or blood cells). They are like blank slates or repair kits that the body can use in a variety of ways.
Immune Cells
Some cell therapies involve reprogramming a person’s own immune cells to help combat diseases such as cancer.
Specialized Cells
In some cases, scientists create or grow cells with a specific purpose, such as insulin-producing cells for diabetes, or dopamine-producing neurons for Parkinson’s disease.
A Brief History of Cell Therapy
Cell therapy is not brand-new. One of the oldest forms of it is the bone marrow transplant, which has been used since the 1950s to treat blood cancers like leukemia. Bone marrow contains stem cells that can grow into healthy blood cells, giving patients a second chance at life.
What’s new today is how much more advanced and precise cell therapy has become. Thanks to breakthroughs in science and technology, we can now grow cells in the lab, edit their genes, and guide them to act in very specific ways inside the body. Some of the most advanced therapies are targeting neurologic diseases like Parkinson’s and ophthalmology conditions that cause blindness.
How Cell Therapy Works
Depending on the disease and the type of therapy, the process can look different. But here are the basic steps:
- Collection: Cells are either taken from the patient (autologous therapy) or from a donor (allogeneic therapy).
- Modification or Culturing: In a lab, scientists grow more of the cells or change them to improve their function — for example, by making them better at targeting cancer cells or by programming them to release helpful proteins.
- Delivery: The cells are injected into the patient’s body — sometimes into the bloodstream, sometimes directly into the affected area (like the eye or the brain).
- Healing: The hope is that the cells will do what they’re designed to do — replace damaged tissue, reset a malfunctioning immune system, or fight disease.
Real-World Uses of Cell Therapy
So, what kinds of conditions are being treated — or might soon be treated — with cell therapy?
Cancer
One of the biggest breakthroughs in recent years is CAR-T cell therapy for blood cancers like leukemia and lymphoma. In this therapy, a patient’s immune cells are taken out, reprogrammed to recognize and kill cancer cells, and then put back into the body. For some patients, this has led to remarkable recoveries after other treatments failed.
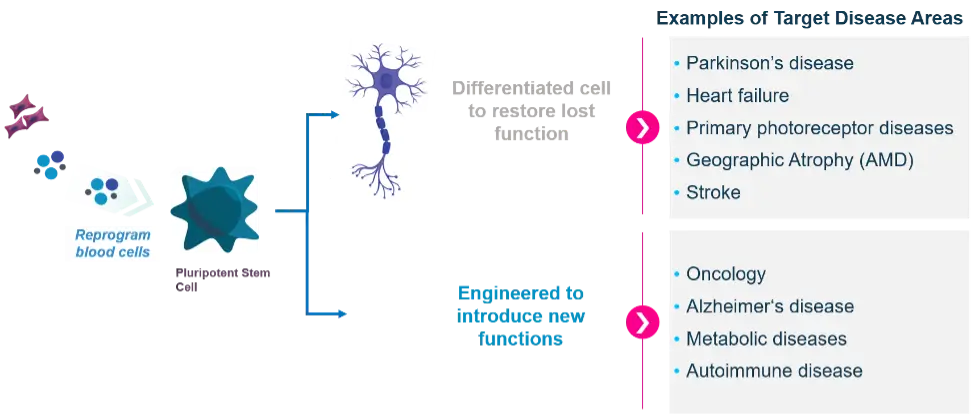
Parkinson’s Disease
This is a brain disorder that affects movement and speech. It’s caused by the loss of specific brain cells that produce a chemical called dopamine. Scientists are now working on transplanting new dopamine-producing cells into patients’ brains, with early signs that this could help improve symptoms and potentially slow the disease.
Eye Diseases
The retina is the part of the eye that allows you to see. Diseases like macular degeneration or retinitis pigmentosa can damage retinal cells, leading to vision loss or blindness. Some cell therapies aim to replace these lost cells, potentially restoring sight for people who had no other options.
Heart Desease
After a heart attack, the heart loses muscle cells that help it pump. Cell therapy aims to regenerate those lost cells, restoring strength to the heart. Although this field is still in early stages, it holds significant promise.
Type 1 Diabetes
This condition occurs when the immune system destroys insulin-producing cells in the pancreas. Cell therapies are being developed to replace these lost cells, helping the body regulate blood sugar naturally—potentially eliminating the need for daily insulin shots.
Benefits of Cell Therapy
- Precision: Cell therapies can be tailored to each individual, especially when using a person’s own cells (autologous cell therapy).
- Long-lasting effects: Some treatments may offer long-term relief or even cures, rather than just symptom management.
- Hope for the untreatable: For many diseases that had few or no options, cell therapy potentially opens new doors.
Challenges and Considerations
With all its promise, cell therapy is still a young and complex field. Here are a few challenges scientists and doctors are working to overcome:
- Safety: Because we’re working with living cells, there’s a need to ensure they don’t grow out of control (like causing tumors) or trigger immune reactions. In addition, cell therapy from donors (allogeneic cell therapy) often requires a period of immune suppression so your body doesn’t reject the new cells.
- Cost: These therapies can be extremely expensive, with some treatments costing hundreds of thousands of dollars. Making them more affordable and accessible is a top priority.
- Manufacturing: Growing and modifying cells in a lab is intricate and scaling it up for large numbers of patients is a big challenge.
- Regulation and Ethics: Because this is a new kind of medicine, governments and scientists must carefully regulate how it’s developed and used—especially when dealing with powerful tools like gene editing.
What’s Next?
The future of cell therapy is bright — and expanding fast. Scientists are exploring its use in many other areas:
- Spinal cord injuries: Repairing nerve cells to restore movement.
- Autoimmune diseases: Resetting the immune system in conditions like lupus or multiple sclerosis.
- Genetic disorders: Using cell therapy alongside gene therapy to correct inherited diseases.
As research progresses, the hope is that cell therapies will move from being rare and cutting-edge to becoming regular tools in hospitals and clinics — much like antibiotics or organ transplants
are today.
What Does It Mean for Patients?
For patients and families, cell therapy represents a powerful kind of hope: the hope that the body can heal from within. The idea of repairing tissues, restoring lost functions, or retraining the immune system — all using living cells — brings us closer to a more personalized and curative form of medicine. Already, some people who once faced terminal illnesses or lifelong disability have seen dramatic improvements. While we are still at the beginning of this journey, the road ahead is full of promise.
In summary:
C}{ell} therapy is an innovative way of treating diseases by using living cells—either your own or from donors—to repair, replace, or reset the body’s systems. It has already transformed treatment for some cancers and is being tested for conditions like Parkinson’s disease, heart failure, vision loss, and diabetes.
Though there are challenges to overcome, especially around safety, cost, and access, the progress being made today suggests that this approach may soon become a cornerstone of 21st-century medicine.
We are witnessing the beginning of a new era—one where healing comes not just from the outside, but from within.
Want to Learn More?
If you’re interested in learning more about cell therapy, talk to your doctor or explore resources from trusted organizations like the National Institutes of Health (NIH), the International Society for Cell & Gene Therapy (ISCT), or patient advocacy groups that focus on your specific condition. Many universities and hospitals also run clinical trials that you can learn about online.
Today’s science fiction is tomorrow’s standard of care. And with cell therapy, the future is already beginning.